 Additionally, the ESC recommends that IVUS should be considered to detect stent related mechanical problems leading to restenosis (Class IIa, level of evidence C) and IVUS should be considered in selected patients to optimize stent implantation (Class IIa, level of evidence B). IVUS for routine lesion assessment is not a recommendation if revascularization with PCI or CABG is not being contemplated (Level of Evidence: C)Įuropean Guidelines have been updated more recently, and the 2018 guidelines from the European Society of Cardiology (ESC) recommends IVUS to assess the severity and optimize the treatment of unprotected left main coronary lesions (Class IIa, level of evidence B).IVUS may be reasonable for the determination of the mechanism of stent thrombosis (Level of Evidence: C).IVUS may be considered for the guidance of coronary stent implantation, especially in cases of left main coronary artery (LMCA) stenting (Level of Evidence: B).IVUS may be reasonable in assessing non–left main coronary arteries possessing angiographically intermediate coronary stenoses (i.e., 50% to 70% diameter stenosis) (Level of Evidence: B).IVUS is a reasonable option to determine the mechanism of stent restenosis (Level of Evidence: C).IVUS and coronary angiography are within reason 4 to 6 weeks and 1-year post cardiac transplantation to rule out donor CAD, detect rapidly progressive cardiac allograft vasculopathy, and provide prognostic information (Level of Evidence: B).IVUS is a reasonable option to assess angiographically indeterminant left main CAD (Level of Evidence: B). 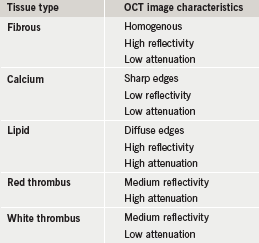
The following are the recommendations made regarding the use of IVUS for PCI, according to guidelines from the American College of Cardiology (ACC). IVUS has indications for a wide range of uses in patients undergoing cardiac catheterization and percutaneous coronary interventions (PCI). For evaluation of stent failure with stent thrombosis or in-stent restenosis, IVUS plays a critical role to identify the mechanism of stent failure, guiding appropriate therapy. IVUS allows for the identification of calcified plaque that may be undetectable from angiography alone. IVUS assessment can distinguish between calcified plaque, lipid, and neointimal proliferation. 
Intravascular imaging with IVUS characterizes and quantifies plaque. The smooth muscle cells comprising the tunica media does not reflect ultrasound waves and appears dark in the gray-scale cross-sectional image, permitting easy identification. Intravascular ultrasound of a coronary artery allows for identification and delineation of the lumen and the 3 layers of the arterial wall: the inner tunica intima, the muscular tunica media, and the outer tunica adventitia. Rather than assessing the vessel from the outside as with angiography, IVUS provides the assessment from within the vessel. This technology overcomes many of the limitations of angiography, which utilizes x-ray technology to produce a 2-dimensional lumenogram of a 3-dimensional structure. Using a dedicated catheter with ultrasound-based technology an image is obtainable from inside an artery producing cross-sectional images with a 360-degree view of the vessel. Intravascular ultrasound (IVUS) is an intravascular imaging modality primarily used in interventional cardiology to characterize lesion morphology, quantify plaque burden, guide stent sizing, assess stent expansion, and identify procedural complications. 
Employ interprofessional team strategies for improving care coordination and communication to advance the diagnosis of coronary artery disease using intravenous ultrasound.Explain the clinical utility of intravenous ultrasound.Describe the indications for intravenous ultrasound.Identify the technique for performing intravenous ultrasound.This activity reviews the role of IVUS and its indications and highlights the role of the interprofessional team in the management of patients with coronary artery disease. Intravascular ultrasound (IVUS) is an intravascular imaging modality primarily used in interventional cardiology to characterize lesion morphology, quantify plaque burden, guide stent sizing, assess stent expansion, and identify procedural complications. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
